 April 2025 Issue
April 2025 Issue
Nutrition for PANS & PANDAS
By Shannon Leatherman, RDN, LDN
Today’s Dietitian
Vol. 27 No. 4 P. 18
The Dietitian’s Role in Improving Patient Outcomes
Most parents describe pediatric acute-onset neuropsychiatric syndrome (PANS)/pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS) “like a light switch went off … one day my child was happy and healthy, and the next day he was paralyzed with fear, shaking his head, angry, aggressive, and afraid to eat.”
What Are PANS & PANDAS?
PANDAS and PANS are chronic, debilitating pediatric neurological disorders first recognized by the medical community in 1998 and 2010, respectively.1,2 Due to the more recent discovery of these illnesses and the ongoing controversy surrounding them,3 many children receive a delayed diagnosis, leading to significant symptom progression.4,5 Currently, research is still evolving as to the best treatment options.6
These disorders are most often characterized by a sudden onset of obsessive-compulsive disorder (OCD), tics, mood and behavior changes, and eating restrictions.1-3 This cluster of symptoms is caused by inflammation of the basal ganglia, the portion of the brain responsible for attention, learning, motor control, executive function, behaviors, and emotions.6,7
For most children, these symptoms progress in a “sawtooth” pattern of flares and remission that can last for months to years. Unfortunately, due to overlapping diagnostic criteria, many children with PANS/PANDAS may be misdiagnosed with pediatric feeding disorder (PFD), avoidant restrictive food intake disorder (ARFID), or other neuropsychiatric disorders, leading to delayed diagnosis and lack of appropriate treatments.7-11
Dietitians can play an important role in both nutrition therapy and advocacy for the treatment of PANS/PANDAS. They may be the first to suggest pursuing a clinical diagnosis after an in-depth patient interview and assessment. RDs can also prevent worsening symptoms by providing early treatment of nutrition-related eating changes and nutrient deficiencies. They can also help patients and their families sort through the safest, best-researched testing and treatment options. Lastly, RDs can assist patients with finding PANS/PANDAS informed providers and support groups for this challenging journey.
Prevalence, Diagnosis, & Common Interventions
PANS and PANDAS are currently considered pediatric clinical diagnoses of exclusion, most commonly occurring in children aged 3 through 13.12,13 PANDAS, a subset of PANS, is estimated to account for 40% to 77% of all PANS cases. According to ASPIRE, a nonprofit dedicated to educating and empowering public and health communities on PANS/PANDAS, the prevalence of PANDAS is estimated to be 1 in 200, with roughly a 3:1 male to female incidence.14 Despite the pediatric diagnostic criteria, there is mounting evidence of adult-onset cases as well.15
Diagnostic Criteria for PANS/PANDAS
Though PANDAS, triggered by group A Streptococcus (GAS), was recognized first, it is a subset of PANS, which does not require a known infectious agent for diagnosis. Both involve diagnostic criteria of abrupt onset of OCD, but other criteria vary slightly between the two diagnoses (see Table 1). What sets these apart from other similar neuropsychiatric conditions is the abrupt onset of primary symptoms along with the accompanying secondary symptoms. For PANDAS, this onset typically occurs within one to three days of an infection, but at times, it can occur 30+ days postinfection.16
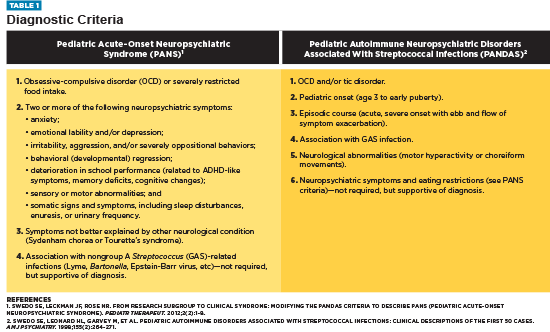
In addition to these clinical signs and symptoms, a thorough medical history, neuropsychiatric evaluation, physical exam, and lab testing can lead to an accurate diagnosis. Since PANDAS is specifically associated with GAS infections, many practitioners use strep tests, including throat cultures, antibody titers, and urine cultures to confirm their suspicions. Doctors diagnosing PANS may test for additional infectious agents.7,16
Physicians who diagnose and treat PANS/PANDAS vary and can overlap between pediatricians, neurologists, immunologists, otolaryngologists, and psychiatrists. However, due to a lack of informed physicians, most parents report seeing an average of eight physicians and waiting an average of three years from the onset of symptoms until receiving a diagnosis for their child.15 The PANDAS Physician Network is a directory of PANS/PANDAS-informed and/or trained physicians that can be a useful reference to potentially guide patients to a quicker diagnosis.
Testing for PANS/PANDAS
To secure a diagnosis of PANDAS, a positive history of GAS infection is necessary. In addition, experts recommend standard lab testing for all newly diagnosed PANS/PANDAS patients to include a complete blood count, comprehensive metabolic panel, erythrocyte sedimentation rate, C-reactive protein, antistreptolysin-O and anti-DNAse B titers, throat cultures, and urinalysis.7,16
For PANS patients, testing for a broader range of infectious agents, including but not limited to Borrelia burgdorferi (Lyme disease), Bartonella, Epstein-Barr virus, and mycoplasma pneumoniae, may also be considered.3 Since PANDAS is an autoimmune condition, testing for vitamin D, thyroid function (including antibodies), celiac, and lupus may be beneficial as well.16 Depending on the patient’s signs and symptoms, some doctors may utilize brain MRIs, electroencephalogram, or swallow studies to assist in their diagnosis and treatment.3,13
Current Treatment Overview
Based on the 2017 Revised Treatment Guidelines for PANS/PANDAS, there is currently a triad of conventional treatment options that includes treating and preventing infections, psychiatric and behavioral interventions, and immunomodulatory therapies.16
Treating and preventing infections most commonly involves the use of antibiotics, both therapeutically and prophylactically. Occasionally, steroids are used during extreme symptom flares.16,17 There’s also limited and conflicting evidence to support tonsillectomies as a beneficial surgical option.16,18
Neuropsychiatric and behavioral treatments involve a combination of psych meds and behavioral therapies to treat the most problematic symptoms. Lastly, immunomodulatory treatments such as intravenous immunoglobulin and plasmapheresis have been shown to be effective; however, the high out-of-pocket cost prevents these from being a plausible option for many patients.6
Because there is currently no known consistent cure for PANS/PANDAS, many families may seek out functional and integrative specialists. These providers tend to run more detailed testing and may also offer the option to include nutrient supplements and herbal antimicrobials as part of their treatment protocols.
Due to an individual’s variable response to conventional treatments and the overwhelming cost of functional medicine, homeopathy has become a popular option for families who have “tried everything.” Anecdotally, many naturopathic doctors and families under their care report full remission with homeopathic remedies, though there’s currently no scientific evidence to support this as a standard of treatment.
Nutrition Implications & Interventions
At this time, there is little to no research published on nutrition therapy standard of care for PANS/PANDAS. The recommendations presented here are a collaboration of research from other neuropsychiatric conditions, OCD, strep-related illnesses, PFD, and eating disorders and are based on the clinical experience of RDs currently treating these conditions.19 Regardless of which method of treatment a patient and their family choose, there are many general and specific nutrition interventions RDs may employ.
PANS/PANDAS Impact on Diet and Nutrition
Due to the OCD involved in all PANS/PANDAS patients, many children regress to very repetitive food choices, fear of certain foods, and fear of germs/food contamination.8 Over time, this repetitive eating selection can lead to nutrient deficiencies and symptoms overlapping with PFD, ARFID, and other eating disorders.9,20 Frequent courses of antibiotics and lack of diet variety also contribute to gut dysbiosis.21
In addition, because of the autoimmune nature of these illnesses, children often experience concurring nutrition-related autoimmune disorders like celiac and thyroid disease, which can impact nutrient absorption and growth patterns. There are also some reports of altered gut function and microbiome composition leading to increased intestinal permeability,21,22 potentially increasing the risk of food allergies and sensitivities in these patients.
PANS/PANDAS Nutrition Assessment
Because of PANS/PANDAS direct and indirect impact on nutrition, it’s essential for RDs to assess changes in growth patterns, nutrient deficiencies, eating behaviors, and gut health. Doing an in-depth evaluation of growth charts can help to target where the child’s goal growth pattern should be and to determine if any catch-up growth is necessary. Completing a thorough food intake assessment and nutrient analysis can help to decipher if any macro- or micronutrients are deficient. Assessing the variety in the child’s diet and screening for PFD and ARFID are also important.
RDs should ask about any food-related behaviors that may impact nutrition, such as fear of choking or food contamination. Including questions about changes in digestive function and sleep provides additional useful information. Doing a nutrition-focused physical exam can validate nutrient deficiencies and the need for further testing and/or supplementation. RDs should also evaluate the patient’s current nutrition-related lab values and medication/supplement regimen for safety and efficacy.
Basic PANS/PANDAS-Focused Nutrition Interventions
Once RDs have pinpointed nutrition problem areas, it’s vital to optimize the patient’s nutrition by preventing malnutrition, supporting special dietary needs, and offering guidance on food patterns and nutrients for brain health, growth, gut health, and immunity. Counseling parents on their role in preventing and reducing picky eating and disordered eating behaviors in their children is also essential.
Since malnutrition exacerbates brain-related feeding challenges, identifying PANS/PANDAS early and providing preventative counseling can be some of the best medicine. RDs can offer parental counseling on the importance of using the Division of Responsibility in their daily feeding practices and on the benefits of continuing to rotate through a variety of foods to avoid fixations.
To support gut and brain health and immune function, PANS/PANDAS patients may benefit from a reduction in heavily processed foods, particularly those low in fiber and antioxidants and high in added sugars, trans fats, and other additives. Helping them transition to a colorful, fiber, healthy fat, and protein-rich diet is a good place to start.19, 23,24
Including protein sources at each meal and snack and optimizing food sources of tryptophan and glycine may improve brain function.19,23 In cases of poor growth, adding in natural energy-rich foods, homemade smoothies, and nutrition shakes is helpful too. Along with dietary changes, most PANS/PANDAS patients may benefit from a high-quality multivitamin and fish oil supplement.19,23,25
If repetitive eating and malnutrition are already underway, the RD can shift goals to preventing further malnutrition and supporting growth restoration. Utilizing more advanced tactics like food chaining and food exposures can be helpful. Referring to speech, occupational, and behavioral therapists may be necessary. In extreme cases, tube feedings may be warranted.
For patients who are working with providers that don’t specialize in PANDAS, dietitians can collaborate by suggesting nutrition-related labs. If any of these values return abnormal, treating the patient with appropriate dietary counseling and nutrient supplementation is vital.
Advanced PANS/PANDAS-Focused Nutrition Interventions
Depending on the patient’s specific symptoms, additional nutrient supplements can be utilized. Probiotic lozenges containing Streptococcus salivarius26 or xylitol-based candies or gums may lower the incidence of recurring oral strep infections.27 N-acetylcysteine and inositol show potential for reducing OCD symptoms for some.28 In addition, ensuring adequacy of nutrients like vitamin C, B6, folate, B12, magnesium, selenium, and zinc may be especially useful in mitigating neurological symptoms and enhancing overall immunity.19,23,28,29
Alongside, improving these patients’ gut health may be vital regardless of overt gastrointestinal symptoms.19,23 Due to the frequent, lengthy courses of antibiotics required for many PANS/PANDAS patients and their impact on the gut-brain axis, probiotics may be beneficial.19,21,23
Greer McGuinness, MS, RD, CDN, CLT, owner of Biomedical Healing for Kids, suggests using individualized probiotics, including “saccharomyces boulardii, broad spectrum or low-histamine,” based on the child’s symptoms and test results.
Many elimination diets have also been studied for both autoimmune and neuropsychiatric conditions.19,23,30 According to one small study, parents of PANS/PANDAS children found gluten-free, casein-free, low-sugar, and anti-inflammatory diets to have the greatest benefits. Parents also report positive behavioral impacts from eliminating specific food additives and any known food allergens or sensitivities.31
Overall, when it comes to counseling these patients on advanced nutrition recommendations, RDs should keep in mind the financial burden of dietary changes and supplements and should offer flexible support. RDs should also consider that OCD and selective eating can be worsened by elimination diets, so these should be used with discretion and careful supervision. McGuinness recommends focusing on “adding foods in to help reduce inflammation” rather than restricting an already limited diet.
RD Advocacy & Support
A final, crucial RD responsibility is the importance of advocating for these patients. Doing a thorough patient assessment can help families put together confusing pieces and pursue a missing diagnosis. Supporting them with compassionate care can also make a big difference. Directing parents to PANS/PANDAS-informed providers, resources, and support groups can set them up for long-term recovery and success.
Often, PANS/PANDAS parents know something isn’t quite right about their child’s cluster of symptoms, but they haven’t found anyone to tie the symptoms together. According to Jessica Setnick, MS, RD, CEDS-C, creator of Eating Disorders Bootcamp (www.eatingdisordersbootcamp.com), if a patient presents with atypical food avoidance or an abrupt onset of ARFID or picky eating, “there’s a high likelihood that PANS could be at play.” Setnick suggests asking targeted screening questions during the patient interview.
She encourages questions such as “Has your child had any diagnosed infections, including strep, mononucleosis, or Lyme in the past year?” McGuiness also includes questions about behaviors such as OCD, tics, bed-wetting, and emotional outbursts. Using good listening skills can help RDs pick up on red flags for PANS/PANDAS. After implementing these screening tools, if you suspect that PANS/PANDAS may be at play, direct the patient to a provider who can provide the proper diagnosis and treatment.
RDs can also provide empathetic care to these patients and their families. PANDAS can be a lengthy and tumultuous journey.32,33 Offer a listening ear, supportive nutrition recommendations, and patience with the parent’s choice and pace of goals.
Finally, patients and parents with PANS/PANDAS often feel isolated and discouraged. Providing them with reputable resources and support groups is essential. These resources can empower parents, validate their concerns, guide them to better treatment options, and reduce their (and their children’s) stress levels.32
Overall, the role of the RD is vital in PANS/PANDAS diagnosis and treatment. RD’s can help bring about change through thorough clinical assessment skills, targeted nutrition interventions, and compassionate and collaborative care.


— Shannon Leatherman, RDN, LDN, is a Quakertown, Pennsylvania-based pediatric and family dietitian. She’s the owner of Food to Table Nutrition, LLC (www.foodtotableRD.com), and a proud PANDAS mom.
References
1. Swedo SE, Leonard HL, Garvey M, et al. Pediatric autoimmune disorders associated with streptococcal infections: clinical descriptions of the first 50 cases. Am J Psychiatry. 1998;155(2):264-271.
2. Swedo SE, Leckman JF, Rose NR. From research subgroup to clinical syndrome: modifying the PANDAS criteria to describe PANS (pediatric acute-onset neuropsychiatric syndrome). Pediatr Therapeut. 2012;2(2):1-8.
3. Prato A, Gulisano M, Scarbo M, Barone R, Vicario CM, Rizzo R. Diagnostic approach to pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (pandas): a narrative review of literature data. Front Pediatr. 2021;9:746639.
4. Arcilla CK, Singla R. Pediatric Autoimmune Neuropsychiatric Disorders Associated With Streptococcal Infections (PANDAS). In: StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2024.
5. O'Dor SL, Homayoun S, Downer OM, Hamel MA, Zagaroli JS, Williams KA. A survey of demographics, symptom course, family history, and barriers to treatment in children with pediatric acute-onset neuropsychiatric disorders and pediatric autoimmune neuropsychiatric disorder associated with streptococcal infections. J Child Adolesc Psychopharmacol. 2022;32(9):476-487.
6. Sigra S, Hesselmark E, Bejerot S. Treatment of pandas and pans: a systematic review. Neurosci Behav Rev. 2018;86:51-65.
7. Swedo S, Menendez CM, Cunningham MW. Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS). In: Ferretti JJ, Stevens DL, Fischetti VA, eds. Streptococcus Pyogenes: Basic Biology to Clinical Manifestations. 2nd ed. Oklahoma City, OK: University of Oklahoma Health Sciences Center; 2022.
8. Toufexis MD, Hommer R, Gerardi DM, et al. Disordered eating and food restrictions in children with PANDAS/PANS. J Child Adolesc Psychopharmacol. 2015;25(1):48-56.
9. Aman M, Coelho JS, Lin B, et al. Prevalence of pediatric acute-onset neuropsychiatric syndrome (PANS) in children and adolescents with eating disorders. J Eat Disord. 2022;10(1):194.
10. Kambanis PE, Thomas JJ. Assessment and treatment of avoidant/restrictive food intake disorder. Curr Psychiatry Rep. 2023;25(2):53-64.
11. Goday PS, Huh SY, Silverman A, et al. Pediatric feeding disorder: consensus definition and conceptual framework. J Pediatr Gastroenterol Nutr. 2019;68(1):124-129.
12. PANDAS questions and answers. National Institute of Mental Health website. https://www.nimh.nih.gov/health/publications/pandas. Updated 2019. Accessed October 12, 2024.
13. Chang K, Frankovich J, Cooperstock M et al. Clinical evaluation of youth with pediatric acute-onset neuropsychiatric syndrome (PANS): recommendations from the 2013 PANS consensus conference. J Child Adolesc Psychopharmacol. 2015; 25(1):3-13.
14. Who gets PANS/PANDAS? Aspire website. https://aspire.care/what-is-pans/who-gets-pans/. Accessed October 12, 2024.
15. Clinical urgency of diagnosing and treating. Aspire website. https://aspire.care/what-is-pans/clinical-urgency-of-diagnosing-treating/. Accessed October 12, 2024.
16. Cooperstock MS, Swedo SE, Pasternack MS, Murphy TK. Clinical management of pediatric acute-onset neuropsychiatric syndrome: part III-treatment and prevention of infections. J Child Adolesc Psychopharmacol. 2017;27(7):594-606.
17. La Bella S, Scorrano G, Rinaldi M, et al. Pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (pandas): myth or reality? The state of the art on a controversial disease. Microorganisms. 2023;11(10):2549.
18. Prasad N, Johng S, Powell D, Williams M, Latimer E, Harley E. Role of tonsillectomy and adenoidectomy in parental satisfaction of treatments for pandas. Am J Otolaryngol. 2021;42(4):102963.
19. Kobliner V. Webinar — Vicki Kobliner — Nutritional Interventions in PANS/PANDAS. Aspire website. https://aspire.care/clinicians/webinar-vicki-kobliner-nutritional-interventions-pans-pandas/. Published September 25, 2022. Accessed October 4, 2022.
20. True G. PANS and eating disorders. Aspire website. https://aspire.care/families-parents-caregivers/pans-eating-disorder-food-restrictions/#. Published July 29, 2021. Accessed October 28, 2024.
21. Quagliariello A, Del Chierico F, Russo A, et al. Gut microbiota profiling and gut-brain crosstalk in children affected by pediatric acute-onset neuropsychiatric syndrome and pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections. Front Microbiol. 2018;9:675.
22. Loffredo L, Spalice A, Salvatori F, et al. Oxidative stress and gut-derived lipopolysaccharides in children affected by paediatric autoimmune neuropsychiatric disorders associated with streptococcal infections. BMC Pediatr. 2020;20(1):127.
23. Strickland E. Eating for Autism. Da Capo Press; 2009.
24. Mazzucca CB, Raineri D, Cappellano G, Chiocchetti A. How to tackle the relationship between autoimmune diseases and diet: well begun is half-done. Nutrients. 2021;13(11):3956.
25. Reimers A, Ljung H. The emerging role of omega-3 fatty acids as a therapeutic option in neuropsychiatric disorders. Ther Adv Psychopharmacol. 2019;9:2045125319858901.
26. Di Pierro F, Colombo M, Zanvit A, Risso P, Rottoli AS. Use of Streptococcus salivarius K12 in the prevention of streptococcal and viral pharyngotonsillitis in children. Drug Healthc Patient Saf. 2014;6:15-20.
27. Kõljalg S, Vaikjärv R, Smidt I, et al. Effect of erythritol and xylitol on Streptococcus pyogenes causing peritonsillar abscesses. Sci Rep. 2021;11(1):15855.
28. Kuygun Karcı C, Gül Celik G. Nutritional and herbal supplements in the treatment of obsessive compulsive disorder. Gen Psychiatr. 2020;33(2):e100159.
29. Gasmi A, Shanaida M, Oleshchuk O, et al. Natural ingredients to improve immunity. Pharmaceuticals (Basel). 2023;16(4):528.
30. Quan L, Xu X, Cui Y, et al. A systematic review and meta-analysis of the benefits of a gluten-free diet and/or casein-free diet for children with autism spectrum disorder. Nutr Rev. 2022;80(5):1237-1246.
31. Khimani K, Abadia-Barrero C, LaRusso M. Implementing dietary changes with children affected by PANS/PANDAS. Child Health Care. 2024;1-19.
32. Ringer N, Roll-Pettersson L. Understanding parental stress among parents of children with paediatric acute-onset neuropsychiatric syndrome (PANS) in Sweden. Int J Qual Stud Health Well-being. 2022;17(1):2080906.
33. McClelland M, Crombez M M, Crombez C, et al. Implications for advanced practice nurses when pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections (PANDAS) is suspected: a qualitative study. J Pediatr Health Care. 2015;29(5):442-452.
